If you’ve been diagnosed with a hiatal hernia, one of the most common questions is whether surgery is necessary.
Most hiatal hernias do not require surgery. Treatment decisions are based on symptoms, size, and whether complications are present.
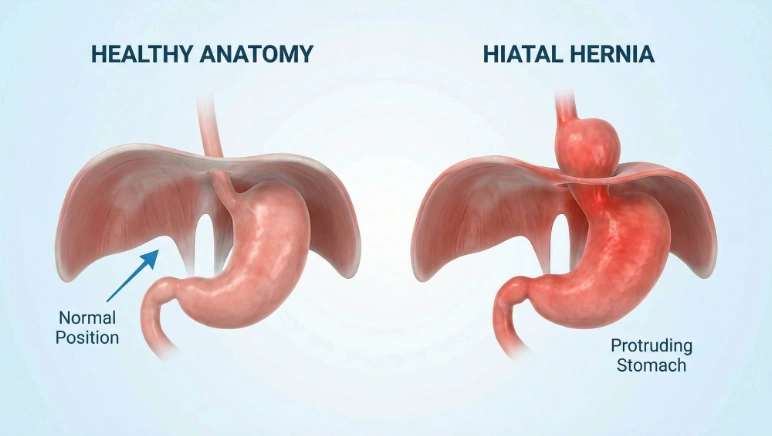
What is a hiatal hernia?
A hiatal hernia occurs when part of the stomach moves up through the diaphragm into the chest.
This can affect how the esophagus and stomach function, often leading to reflux symptoms like heartburn or regurgitation.
Types of hiatal hernias
Sliding hiatal hernia
This is the most common type, accounting for about 95% of cases.
- The stomach and esophagus move up into the chest
- Often associated with acid reflux (GERD)
- Symptoms may come and go
Paraesophageal hiatal hernia
Less common, but more serious.
- The stomach pushes next to the esophagus
- The stomach can become trapped in the chest
- Higher risk of complications like obstruction or reduced blood flow
Does the size of a hiatal hernia matter?
Yes, but size alone does not determine the need for surgery.
Hiatal hernias are often described as:
- Small: Often no symptoms or mild reflux
- Moderate: May cause more noticeable symptoms
- Large: More likely to cause significant symptoms or complications
Larger hernias are more likely to require surgical evaluation, but the decision depends on the full clinical picture.
When is surgery recommended for a hiatal hernia?
Surgery is typically considered when symptoms are not controlled with medication or when complications develop.
Common reasons for surgery
Persistent or severe symptoms
- Ongoing heartburn or reflux despite treatment
- Difficulty swallowing
- Chest discomfort or pressure
Complications
- Paraesophageal hernia
- Stomach becoming trapped (incarceration)
- Reduced blood supply (strangulation)
- Chronic anemia or bleeding
- Barrett’s esophagus in select cases
Quality of life concerns
- Long-term dependence on medications
- Symptoms interfering with daily activities
How is a hiatal hernia evaluated?
Your provider may use imaging and endoscopic tests to confirm the diagnosis and assess severity.
Common tests include
- Barium swallow (X-ray): Shows how the stomach and esophagus move
- CT scan: Provides detailed images of the hernia
- Upper endoscopy (EGD): Examines the esophagus and stomach lining
- pH or motility testing: Evaluates reflux and esophageal function
These tests help guide treatment decisions.
Surgical options for hiatal hernia repair
When surgery is recommended, most procedures aim to return the stomach to its normal position and repair the diaphragm opening.
Minimally invasive (laparoscopic or robotic) repair
- Small incisions with camera guidance
- Shorter recovery time
- Less postoperative pain
Open repair surgery
- Larger incision
- Used for complex or very large hernias
- May be necessary in certain cases
Our hernia surgeon will recommend the best approach based on your condition.
Is surgery always necessary?
No. Many hiatal hernias are managed without surgery.
Lifestyle changes and medications often help control symptoms:
- avoiding trigger foods
- eating smaller meals
- not lying down after eating
- using acid-reducing medications
Surgery is usually reserved for cases where these measures are not enough.
When should you see a specialist?
You should consider evaluation if you have:
- frequent or severe reflux symptoms
- trouble swallowing
- chest or upper abdominal discomfort
- symptoms that do not improve with medication
Early evaluation can help prevent complications and clarify whether surgery is appropriate.
Take the next step
If you are dealing with symptoms of a hiatal hernia or have been told you may need surgery, a specialist evaluation can help you understand your options.
Call (925) 940-1025 or request a consultation with Hernia Innovations.